Periodontal disease affects nearly half of adults worldwide and remains one of the leading causes of tooth loss. Traditionally, treatment has focused on removing plaque and killing bacteria through deep cleaning, antiseptics, and antibiotics.
But there’s a problem.
Harmful bacteria don’t act alone – and wiping out all bacteria often creates the perfect conditions for them to come roaring back.
Emerging research suggests a smarter strategy: working with beneficial bacteria, not against them.

Periodontal Disease Is a Microbial Imbalance (not an infection)
Periodontitis is caused by bacteria, but not in the way we once thought.
Research shows that so-called “periodontal pathogens” (such as Porphyromonas gingivalis) are present in both healthy mouths and diseased ones. The difference isn’t their presence – it’s their dominance.
When harmful bacteria overwhelm beneficial species, inflammation follows. Over time, this inflammatory response damages gums, connective tissue, and bone.
This reframes periodontal disease as a problem of microbial imbalance, not simply poor hygiene.
Why Conventional Treatments Fall Short
Standard periodontal therapies — scaling, root planing, antiseptics, and antibiotics — can be effective in the short term. However, they have clear limitations:
- They remove beneficial bacteria along with harmful ones
- Pathogens often recolonise treated sites
- Antibiotic resistance is an increasing concern
- Long-term disease management relies heavily on repeated intervention
In short: we’re good at clearing the battlefield, but not at rebuilding it.
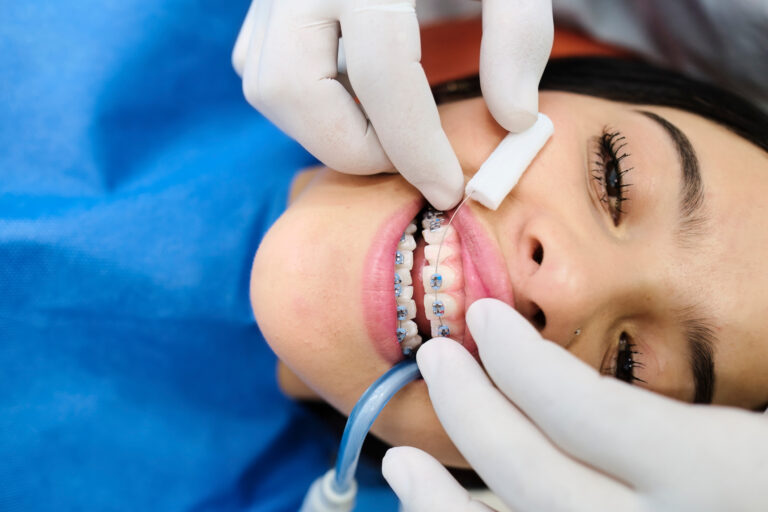
What Are Probiotics in Oral Health?
According to the World Health Organization, probiotics are “live microorganisms which, when administered in adequate amounts, confer a health benefit on the host.”
In oral health, probiotics are typically delivered through:
- Lozenges
- Chewing gum
- Powders
Unlike antibiotics, probiotics don’t aim to sterilise the mouth. Instead, they support oral health by competing with pathogens and calming inflammation.
How Probiotics May Help Gum Health
The review highlights several mechanisms by which oral probiotics may support periodontal health:
1. Inhibiting Harmful Bacteria
Certain probiotic strains produce bacteriocins and other antimicrobial substances that suppress periodontal pathogens and interfere with plaque biofilm formation.
2. Competing for Space
Probiotics can adhere to oral tissues and dental surfaces, making it harder for harmful bacteria to colonise.
3. Reducing Inflammation
Some strains reduce inflammatory mediators such as matrix metalloproteinases (MMPs) and prostaglandins, which are linked to tissue destruction in periodontitis.
4. Supporting Bone Health
Fermentation by specific probiotic strains can generate bioactive peptides that stimulate bone-forming cells, potentially helping counter bone loss associated with advanced periodontal disease.
Evidence Across Key Oral Conditions
Gingivitis
Clinical studies reviewed showed that probiotic strains such as Lactobacillus reuteri and Lactobacillus casei were associated with:
- Reduced gingival inflammation
- Lower enzyme activity linked to tissue breakdown
Periodontitis
Healthy individuals were found to naturally harbour higher levels of beneficial lactobacilli and bifidobacteria compared to those with chronic periodontitis, suggesting these bacteria play a role in maintaining oral balance.
Halitosis
Probiotics showed particularly strong promise in managing bad breath. Strains such as Streptococcus salivarius K12 reduced volatile sulphur compounds – the primary cause of oral malodour more sustainably than chemical mouthwashes.
Bacterial Replacement Therapy: A Bigger Idea
While probiotics offer temporary support, bacterial replacement therapy aims for something more ambitious: long-term microbiome change.
Instead of ingesting bacteria, clinicians directly introduce beneficial strains into periodontal pockets after cleaning. Animal studies demonstrated:
- Reduced pocket depth
- Less bleeding
- Improved attachment levels
- Increased bone density
This approach is based on “guided recolonisation”. Deliberately rebuilding the oral ecosystem with health-associated bacteria.
Although still experimental, it represents a fundamental shift in periodontal treatment philosophy.
What This Means for the Future of Oral Care
The key insight from this research is simple but powerful:
Periodontal disease may be better managed by engineering a healthy oral microbiome, rather than repeatedly destroying it.
Probiotics are not a replacement for brushing, flossing, or professional care – but they may become valuable adjuncts in long-term gum health strategies.
Bacterial replacement therapy, while still in early stages, points to a future where dentists actively design healthier oral ecosystems.
The Bottom Line
- Periodontal disease is driven by microbial imbalance and inflammation
- Probiotics can help rebalance the oral microbiome and reduce inflammation
- Benefits are strain-specific and often require continued use
- Bacterial replacement therapy shows promise for longer-lasting effects, but needs further clinical validation
As oral health science evolves, one thing is clear: the future isn’t about killing bacteria, it’s about choosing the right ones.